Clinical Passion Deserves a Conversation Before It Deserves a Committee
A clinician has an idea. Something they have seen in their ward, their clinic, their theatre, that could be better. A workflow that wastes time, a gap in care, a tool that does not yet exist, a process that has not caught up with what is now possible. The idea comes from exactly where healthcare improvement is supposed to come from: someone who does the work, every day, seeing what nobody who does not do the work can see.
They take the idea home. They think about it in the car. They sketch it on the back of an envelope. They start researching products, drawing processes, writing notes. Somewhere between week three and month six, they have invested enough of themselves that it is no longer just an idea. It is their idea. It matters to them.
And then, often, it dies. Not because the passion was wrong, but because three things happened that were almost impossible to see from inside the idea. The product the clinician settled on turned out to be solving a related problem, not quite this one. Someone else, in another directorate or another trust, had already spent a year building something very similar. A constraint that looked small from outside turned out to be fatal from inside.
The idea is quietly shelved. The clinician absorbs the loss. Nobody in the organisation sees the total cost, because the cost was borne privately, over evenings and weekends, in emotional investment that is now recoverable only as fatigue or cynicism.
This is passion waste in healthcare, and the thing that prevents it is not more process. It is a conversation that should have happened six months earlier.
The Real Problem Is Isolation
Clinical innovators, in most organisations, have nowhere safe to have an early conversation about an idea. Sharing with a line manager risks being told to stop because of workload. Sharing with a formal committee risks triggering a review the idea is not ready for. Sharing with colleagues over coffee produces polite encouragement but rarely the specific information that would actually help. Sharing with digital or research colleagues feels presumptuous until the idea is more developed, and by the time the idea is more developed, the cost of changing direction has risen enough that sharing becomes defensive rather than exploratory.
So the clinician does what capable, committed people always do. They push forward alone, on their own time, with the information they have. Or so they think, or will often declare, but the idea is creeping into daily activities, influencing decisions. And the information they have is almost always incomplete, because the information that would have helped most is sitting with somebody they have never met, in a part of the organisation they have no reason to visit.
This is not a failure of clinical behaviour. It is a failure of organisational design. The absence of a place to have the right conversation, early, with the right people, is not a neutral condition. It is what turns clinical passion into wasted effort.
What a Peer Review Platform Actually Does
A clinical innovation communications platform is, at its core, that early conversation, made available to anyone who wants to start one. It is not a governance layer. It is the opposite. It is an accelerator for passionate people.
Its shape is simple. A clinician posts an early idea, in their own language, with a clear description of the patient problem they want to solve and the direction they are thinking of taking. Other clinicians, digital colleagues, researchers, and subject experts respond, quickly and constructively. Some responses confirm the idea is worth pursuing. Some point to prior work that saves the clinician months. Some surface a practical wrinkle the originator could not have seen from inside the idea. Some connect two people who turn out to be thinking the same thing independently.
The value is not in any single response. The value is in the aggregation. A well-designed platform gives a clinician, in a week or two, the kind of feedback it would have taken them six months to assemble on their own.
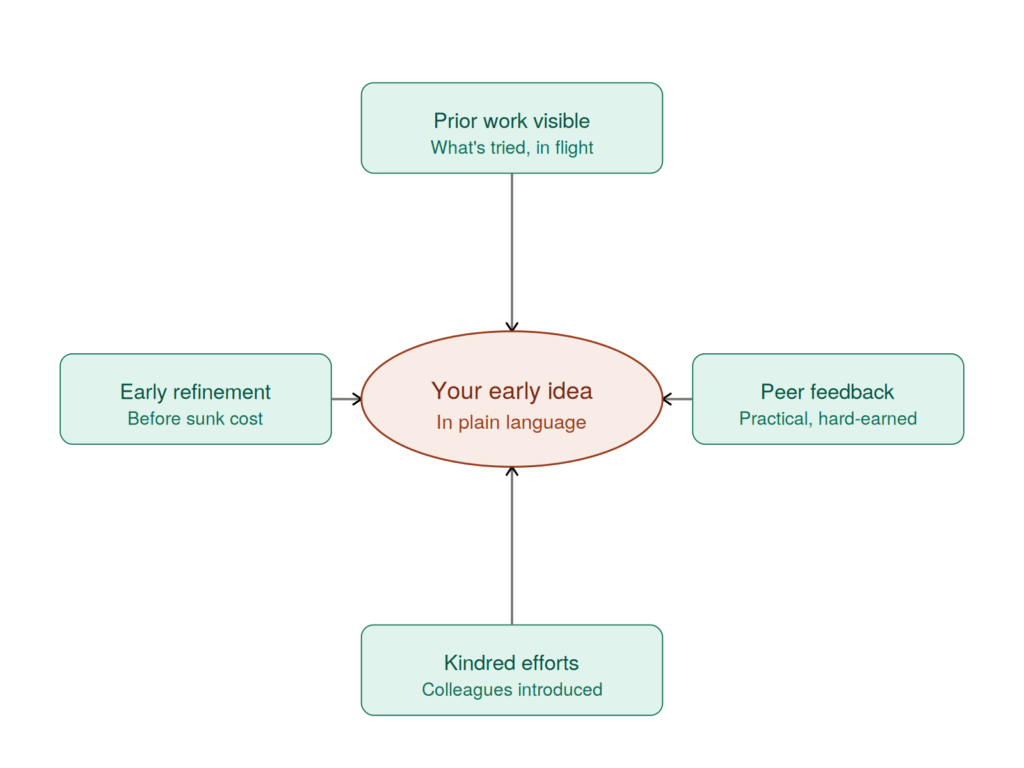
In practical terms, the platform does four things that matter to the innovator directly.
It makes prior work visible. The single most frustrating moment in any clinician’s innovation journey is the discovery, usually late, that the same idea has been tried before, or is being tried now, by someone they could have talked to. A searchable record of what has been attempted, what is in progress, and what colleagues have proposed prevents this almost entirely. Not as a gate, but as a gift.
It produces constructive early feedback. Peers who have tried adjacent ideas know things that cannot be learned from searching. The nurse who tried a similar workflow and found it did not survive out-of-hours staffing. The allied health professional who discovered the vendor’s tool only worked on a browser the trust does not support. The registrar who piloted something like this in a different directorate and learned where it breaks. This is not objection. It is hard-earned experience, offered generously, and it is the most valuable input an early idea can receive.
It connects people who are thinking the same thing. When two clinicians are working on the same problem, separately, the platform introduces them. The waste of two parallel efforts becomes the momentum of one combined one. This almost never happens in the current default, because the two clinicians have no way of knowing the other exists.
It allows ideas to be refined or retired well. Not every idea survives peer review, and that is the point. An idea refined early, with clear input from colleagues the clinician respects, is an entirely different experience from an idea ground down later by a process the clinician does not know. The first is a collaboration; the second is a rejection. A good platform makes the first possible at the point where it would be most useful.
Why This Respects Clinical Passion Rather Than Limiting It
The instinctive concern, when platforms like this are proposed, is that they will slow innovation down or create new barriers. The opposite is true. The current default, in which passionate clinicians work in isolation and only discover the problems with their ideas after significant personal investment, is the slow path. Peer review, done well, is the fast one.
A clinician whose early idea gets connected, within a fortnight, to three colleagues working on related problems has not been slowed down. They have been given a year of momentum they would otherwise have spent alone. A clinician whose early idea gets a considered response explaining why a particular product will not quite work, with a suggestion of two alternatives that might, has not been blocked. They have been given information that would otherwise have cost them six months to acquire the hard way.
The platform is respectful because it assumes the clinician is entirely capable of using good information well. It treats the innovator as someone who would make better decisions with better input, and then supplies the input. That is a different relationship from one in which the innovator is assessed by committees after the fact.
What This Requires From Organisations
Building the technology is not hard. A searchable space, a structured way to post an early idea, a norm of quick constructive response, a simple mechanism for matching similar ideas. The engineering is trivial.
The cultural commitment is harder, and it is where most organisations fall short. Responses have to be quick enough that clinicians use the platform before they have privately committed. Feedback has to be honest enough to be useful and generous enough not to wound. Ideas that are set aside have to be set aside with reasoning, from peers, not with silence from a mailbox. And clinicians who post an idea that turns out to be duplicative or unfeasible have to be actively thanked for posting early, not quietly remembered as someone whose idea did not work. The posting is the good behaviour. That has to be what gets recognised.
Organisations that get this right produce clinicians who share earlier, test faster, and burn far less of their own time on ideas that were never going to ship. Organisations that get it wrong produce the pattern we already have.
The Human Stakes
Clinical passion is not a renewable resource. Every clinician who invests six months of unpaid effort in an idea that quietly dies is a clinician who is a little less likely to invest the next six months. The cost is not borne by the organisation in any line it can see. It is borne by the clinician, and by the patients who would have benefited from the next idea that clinician will now not have.
The case for peer review platforms in healthcare is not a governance case. It is a human one. Passionate people deserve information before they deserve committees. They deserve colleagues before they deserve processes. They deserve a conversation at the start, not a judgement at the end.
The organisations that build this infrastructure protect the thing healthcare cannot afford to lose. The organisations that do not are quietly losing it already, one unseen idea at a time.
